Transcript of Q&A
Treatment Options for Acoustic Neuromas, a Common Brain Tumor
 Acoustic neuromas are benign tumors that cause hearing loss, tinnitus, and dizziness. They are one of the most common brain tumors diagnosed in the United States, which translates to about 3,000 new cases each year. Several treatments are available for these tumors, depending on the size of the tumor, symptoms, patient age and overall health.
Acoustic neuromas are benign tumors that cause hearing loss, tinnitus, and dizziness. They are one of the most common brain tumors diagnosed in the United States, which translates to about 3,000 new cases each year. Several treatments are available for these tumors, depending on the size of the tumor, symptoms, patient age and overall health.
For more than 20 years, George Wanna, MD, Executive Vice Chair of Otolaryngology – Head and Neck Surgery and Chief of the Division of Otology-Neurotology at the Mount Sinai Health System, has specialized in the surgical management of acoustic neuromas. He has performed approximately 1,000 procedures to treat these unusual tumors and improve the quality of life of his patients.
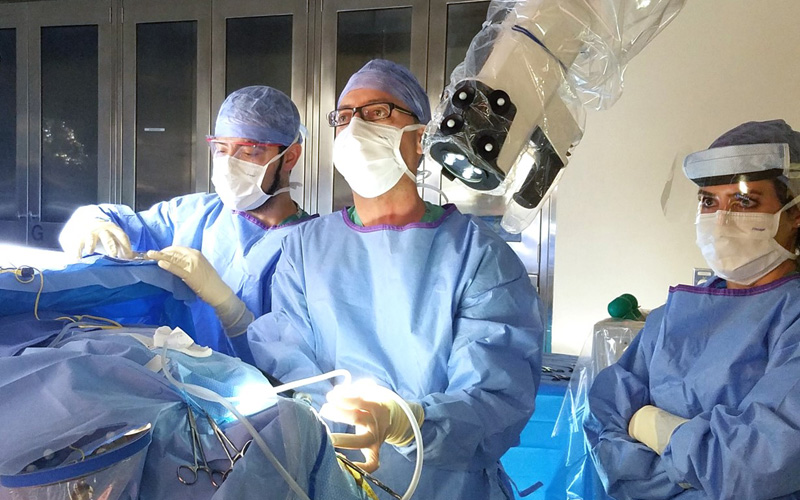
Acoustic neuromas can be treated surgically in a variety of ways. As a pioneer in the field, Dr. Wanna specializes in several approaches, including removal of the tumor endoscopically through the ear canal. Dr. Wanna was one of the first skull base surgeons to use the exoscope, or a robotically controlled microscope. The exoscope offers surgeons increased visualization with high-definition, real-time imagery.
In this Q&A, Dr. Wanna explains the various treatment options for acoustic neuromas, and he answers common questions about the benefits of endoscopic surgery, the use of radiation, and how the exoscope can improve outcomes for patients.
How is acoustic neuroma removed endoscopically? How is this surgery different from conventional, “open” surgery?
An endoscopic approach allows us to access the tumor through the ear canal without any major incisions. The endoscope is a thin, rigid tool with a light and high-definition camera attached to the end. We use it to look through the ear canal, behind the ear drum and inner ear, and into the brain. It can be our main surgical tool or used in combination with open surgical techniques that require an incision. Often the endoscope will allow for a more minimally invasive approach, even when used as an adjunct in open surgery.
What are the benefits of using an endoscopic approach?
There are no major incisions. The procedure is done entirely through the ear canal. Patients who have endoscopic surgery recover faster and typically go home within 48 hours.
Who is a candidate for endoscopic surgery?
Every case is different, and it is important to individualize the approach to each patient with the goal being to treat the tumor in the safest, most effective way. Patients with small tumors who have lost their hearing are ideal candidates for endoscopic techniques. Conventional, open surgical approaches are used to treat larger tumors in deeper locations. In some cases, a wait-and-see approach is taken for patients with smaller tumors and good hearing, or those with stable tumors. Typically, we do not operate on small, stable tumors (less than 1 cm). However, if the tumor is growing and the patient prefers it to be removed, we may perform surgery earlier than expected.
How do you know the size of the tumor?
We assess tumor growth using MRI scans. We measure the tumor in 3 dimensions and compare each dimension and overall volume from scan to scan. These measurements are then used to help guide decision making along with the patient.
Does endoscopic surgery reduce potential side effects like facial paralysis or cerebrospinal fluid (CSF) leak?
At Mount Sinai, we have extremely high success rates with endoscopic surgery and were one of the first adopters of the technology in ear surgery. Asone of the highest volume endoscopic ear surgery centers in the world, we have adapted our experience to acoustic neuroma surgery. For example, we have found that packing the Eustachian tube under direct visualization reduces the risk of CSF leaks. In essence, we employ the principles of conventional, safe surgery and use the endoscope to accomplish the same goals in a minimally invasive approach.
Is radiation used after surgery? Does everyone need it?
This is a vibrant discussion in the field of otology-neurotology. Radiation is used in certain patients, If the tumor is large and pressing on the brainstem, surgery is most appropriate. Radiation should only be used when there is MRI documentation of tumor growth and can be the treatment of choice for elderly patients or those with other existing comorbidities. In some cases, the acoustic neuroma cannot be completely removed without causing facial paralysis; in those cases, a very small remnant is purposefully left behind, and if it grows, is radiated.
What is the exoscope? How does it help surgeons visualize the tumor?
The exoscope is a specialized microscope with a robotic arm. It can generate 2D or 3D images and is guided by voice command. It has a built-in surgical GPS which allows us to see in real time on a CT scan or MRI exactly where we are. This exceptional visualization of the patient’s anatomical structures is unprecedented.
What are the benefits of coming to the Ear Institute of New York Eye and Ear Infirmary of Mount Sinai?
While acoustic neuromas are relatively uncommon, we are one of the highest volume centers in the country, giving patients the advantage of seeing providers who have treated the full spectrum of these tumors, including the most complex cases. We work very closely with our colleagues in neurosurgery and radiation oncology to ensure patients receive the most appropriate and optimal treatmentfor them. Our extensive support staff guides patients through every step of the way.
What are the benefit of collaboration between surgeons and trainees at the Ear Institute?
The exoscope projects a real-time, high quality display of anatomical images that both neurosurgeons and otologists can view simultaneously, rather than individually through a microscope. This creates a true collaborative approach between surgeons and anesthesiologists, as well as for other medical experts (domestic and international), who may be observing the procedure. This technology has also greatly enhanced the educational experience at the Icahn School of Medicine at Mount Sinai for residents, fellows and medical students, as we continuously harness innovative technology for the next generation of surgeons.
To make an appointment with Dr. Wanna at the Ear Institute of New York Eye and Ear Infirmary of Mount Sinai, please call 212-979-4200
Acoustic Neuroma Removal at Mount Sinai
- Steven Nordman
 I was traveling a lot for work in 2015 when I noticed I was blinking a lot. Associates noted it looked like I had a nervous tic. Some suggested I might want to reduce caffeine – I enjoy my cup of strong coffee. I went to doctors and had some tests done. I learned I had blepharospasm (benign essential blepharospasm) – a type of dystonia or movement disorder, which can be treated by Botox injections to control it.
I was traveling a lot for work in 2015 when I noticed I was blinking a lot. Associates noted it looked like I had a nervous tic. Some suggested I might want to reduce caffeine – I enjoy my cup of strong coffee. I went to doctors and had some tests done. I learned I had blepharospasm (benign essential blepharospasm) – a type of dystonia or movement disorder, which can be treated by Botox injections to control it.
At that time, I underwent an MRI of my head in January 2016 when it was discovered I had a “lesion” on my brain. It was an “incidental finding”. I was told I was lucky it was discovered. It’s hard to equate “being lucky” with discovering you have a brain tumor, but this is how the story goes. Later I would understand that it was a small brain tumor – about a half inch in size. It was technically an acoustic neuroma (also called a vestibular schwannoma), and it was very slow growing – so I probably had it for 7-10 years and never knew about it.
I had no pain and no symptoms, except my hearing on that side was decreasing, which I attributed to aging (being in my 50s). I could leave it alone and observe it, or I could have it physically extracted (invasive surgery – cranial/brain surgery), or I could zap it (stereotactic radiation), which should inactivate it and stop any growth. The stereotactic radio surgery seemed the optimal move – plus it had a 95% success rate. So that is the route I chose. There was a 50% chance of loss of hearing on the side where the neuroma was, but I accepted that risk.
Semi annual and annual MRIs revealed no change in tumor size – all good – until my annual checkup in January 2019. That’s when it doubled in size to about an inch. It went from small to large, in an area of your brain where there is not a lot of free space. It started pressing on my brain stem, causing some facial numbness, some balance issues, and 80% loss of hearing on the left side. I guess 95% successful means 5% of the time it does not work – so the math is the math. I fell in the 5% and urgently needed to address my now large brain tumor.
I had an appointment with a number of neurosurgeons at the time throughout NYC and Mount Sinai’s skull base surgeons really impressed me both with their knowledge of my condition and their experience in performing this type of surgery. Deciding to have brain surgery – cranial surgery – is a scary proposition, and not easily arrived at. When I first met with Dr. Joshua Bederson I had heard of his fantastic reputation and he lived up to all expectations. He is a brilliant and experienced cranial surgeon – and he and his team made me totally comfortable with what was a very scary process for someone who had no experience with dealing with having to have brain surgery.
I met with Dr. George Wanna, an expert ENT/otolaryngologist, for my hearing loss, and when I decided to have the surgery done at Mount Sinai, he was an integral part of my surgical team. His communication skills, knowledge, background, expertise, compassion and willingness to listen and explain everything to someone without a medical background, made Dr. Wanna an easy choice for me. He made a very difficult decision easier, and his after care and support, as well as his staff’s kindness, made my procedure and follow-up care go smooth as glass. I am six weeks removed from my surgery and I feel great and better and stronger every day. I was home from the hospital in five days and I am back to work and feeling great.
I strongly recommend anyone needing attention for an acoustic neuroma to see Dr. George Wanna and Dr. Joshua Bederson at Mount Sinai’s Skull Base Surgery Center. I received gold level service and am happy to have been able to locate them and the surgical team at Mount Sinai and New York Eye and Ear Infirmary of Mount Sinai and the brilliant work that they do.
If anyone is going through this daunting process my advice to you is get several opinions from top doctors and hospitals and get comfortable with your hospital and the medical team that you will be selecting to do the surgery and aftercare. The studies show experience counts on these procedures and leads to improving your chance for success. I am very happy to have gone through this process with Mount Sinai and recommend them to you.

































